Reproductive Health
Cervical Stenosis: An Overlooked Cause of Period Pain?
Is Your Period Pain More Than Just "Bad Cramps"?
For many women, the monthly menstrual period is synonymous with some degree of pain. Mild to moderate cramps are a common experience, and for some, the discomfort escalates to the severe, debilitating pain of dysmenorrhea, often attributed to conditions like Premenstrual Syndrome (PMS) or its more intense counterpart, Premenstrual Dysphoric Disorder (PMDD).
However, what if your excruciating period pain, or even unusually light periods, is signalling an underlying physical issue that's often overlooked?
Enter cervical stenosis. This gynaecological condition, characterized by a narrowing or even complete closure of the cervical canal, can be a hidden culprit behind severe menstrual pain.
Its symptoms are sometimes mistakenly attributed to hormonal imbalances or psychological distress. Understanding cervical stenosis can be the key to finally getting answers and relief for your perplexing menstrual symptoms.
What Exactly is Cervical Stenosis?
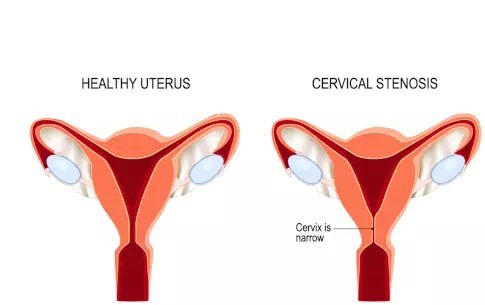
The cervix is the lower, narrow part of the uterus that connects to the vagina. It has a small opening, the endocervical canal, through which menstrual blood flows out and sperm can enter. Cervical stenosis occurs when this canal becomes abnormally narrowed or completely blocked.
Why does Cervical Stenosis Happen?
Congenital: Some women are born with a naturally narrow cervix.
Acquired: This is more common and can result from:
Gynaecological Procedures: Most frequently, procedures like a LEEP (Loop Electrosurgical Excision Procedure) or cone biopsy performed to treat abnormal cervical cells, or endometrial ablation (a procedure to reduce heavy menstrual bleeding), can cause scarring that leads to stenosis (Dr. Thais Aliabadi, n.d.).
Infection or Inflammation: Chronic infections or inflammation of the cervix can lead to scarring and narrowing.
Radiation Therapy: Treatment for pelvic cancers can cause scarring.
Cervical Atrophy: In postmenopausal women, the cervical opening can naturally narrow due to declining estrogen levels.
Rarely, Cervical Cancer: Though less common, a tumor can cause obstruction.
While cervical stenosis might be asymptomatic, particularly in postmenopausal women, its impact on premenopausal women with an active menstrual cycle can be profound.
The Direct Impact: How Cervical Stenosis Causes Severe Period Pain
The most direct and significant consequence of cervical stenosis in premenopausal women is severe menstrual pain, or dysmenorrhea. Here's the mechanism:
Blocked Outflow: If this pathway of the cervical canal is too narrow or blocked, the blood that needs to exit the uterus, gets trapped inside the uterus.
Increased Uterine Pressure and Contractions: When blood cannot escape efficiently, pressure builds up within the uterine cavity. The uterus then responds by contracting more forcefully and intensely to try and expel the trapped blood. These powerful, often spasmodic, contractions are the source of the excruciating pain (Nova IVF Fertility, n.d.).
Hematometra: The accumulation of menstrual blood inside the uterus is called hematometra. This condition not only causes severe pain but can also lead to uterine distension and discomfort.
Retrograde Menstruation: If the path forward is blocked, menstrual blood can be forced backward, traveling up the fallopian tubes and into the pelvic cavity. While some retrograde menstruation is normal, excessive backward flow can increase the risk of endometriosis, a condition where uterine-like tissue grows outside the uterus. Endometriosis itself is a significant cause of chronic pelvic pain and severe dysmenorrhea, creating a compounding effect on pain (Dr. Thais Aliabadi, n.d.).
Inflammation: The trapped blood and increased pressure can also contribute to inflammation within the uterus and surrounding pelvic structures, further intensifying the pain.
The Indirect Link: Cervical Stenosis and PMS/PMDD Confusion
Cervical stenosis doesn't directly cause hormonal imbalances or the neurobiological sensitivities linked to PMS and PMDD. However, the sheer burden of severe, chronic, or recurrent pain can significantly impact mental and emotional well-being, often leading to symptoms that mimic or exacerbate those seen in PMS or PMDD.
Pain-Induced Stress: Chronic pain can disrupt sleep, increase anxiety, lead to feelings of frustration, helplessness, and depression, and generally reduce one's capacity to cope with daily life (Verywell Health, n.d.).
Exacerbated Mood Symptoms: For someone already predisposed to PMDD, the added layer of severe physical pain can push their emotional symptoms to an unbearable level.
Sleep Deprivation: Intense pain often leads to poor sleep, which is a known exacerbator of mood disturbances, fatigue, and cognitive difficulties, all common in PMDD.
Impact on Daily Functioning: Both PMDD and severe dysmenorrhea from cervical stenosis can prevent one from working, socializing, or engaging in usual activities. This isolation and functional impairment can further contribute to feelings of depression and anxiety, blurring the lines between physical and emotional distress.
Diagnostic Misattribution: Because both conditions cause significant distress around the menstrual period, severe pain from undiagnosed cervical stenosis might be mistakenly attributed solely to "bad PMS" or PMDD. This can lead to ineffective treatment strategies that only address the mood symptoms, leaving the underlying physical cause unaddressed.
Recognizing the Signs and Seeking Diagnosis
If you experience unusually severe period pain that doesn't respond to typical pain relief, significantly lighter periods than usual, absent periods (in the absence of pregnancy), or chronic pelvic pain, especially after a cervical procedure, it's crucial to discuss cervical stenosis with your gynaecologist.
Diagnosis typically involves:
Pelvic Exam: Your doctor may note difficulty passing instruments through the cervix.
Uterine Sounding: Attempting to pass a small, thin rod through the cervix into the uterus.
Ultrasound: To check for fluid or blood build-up in the uterus (hematometra).
Hysteroscopy: A procedure where a thin, lighted scope is inserted through the cervix to visualize the canal directly and identify the narrowing or scarring.
Treatment for Cervical Stenosis
The primary treatment for cervical stenosis is cervical dilation. This involves using a series of progressively larger rods (dilators) to gently widen the cervical canal. In some cases, a small tube or stent may be placed temporarily to help keep the canal open. If scar tissue is significant, hysteroscopic resection (surgical removal of scar tissue) may be performed.
Once the cervical opening is restored, menstrual blood can flow freely, and the severe, obstructive period pain typically resolves. This relief from physical agony can, in turn, significantly improve overall well-being and potentially reduce the intensity of any co-existing PMS or PMDD symptoms by reducing the chronic stress burden on the body.
Related Articles
Understanding the various facets of your reproductive health is key to effective management. Explore these related articles on HealCycle for further insights:
What Treatments are Available for My PMDD Symptoms?: If cervical stenosis is ruled out or addressed, this resource can help you explore effective strategies for managing confirmed PMDD.
How Do My Hormones Make Me Feel So Up and Down?: While cervical stenosis is structural, the compounded stress and pain it causes can amplify hormonal sensitivities, making this article relevant for understanding the brain-body connection.
Conclusion
Cervical stenosis is a physical condition that can be an overlooked yet significant cause of severe menstrual pain, often leading to symptoms that mimic severe PMS or PMDD. The excruciating pain arises from the obstruction of menstrual blood flow. While it doesn't directly cause hormonal mood disorders, the chronic pain and distress it inflicts can undeniably worsen psychological well-being. If your period pain is unusually severe, constant, or accompanied by very light or absent periods, it's crucial to seek a thorough evaluation from your gynaecologist.
Disclaimer:
The information provided in this blog post is for informational purposes only and does not constitute medical advice. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your qualified healthcare provider with any questions you may have regarding a medical condition or before starting any new treatment or making any changes to existing medical care.
References
Dr. Thais Aliabadi. (n.d.). Cervical Stenosis. Dr. Thais Aliabadi.
Healthline. (n.d.). Closed Cervix: What Does it Mean If I'm Not Pregnant?. Healthline.
Nova IVF Fertility. (n.d.). What are The Best Treatments for Cervical Stenosis?. Nova IVF Fertility.
Verywell Health. (n.d.). What Causes Lower Back Pain in Females?. Verywell Health.
Latest
From the Blog
Discover fresh insights, practical tips, and empowering stories to help you learn and grow in your PMDD healing journey. We're always here to remind you that you're not alone




