Periods, Products
Can Your Pad Really Detect Disease? The Truth About MenstruAI
Imagine a future where your menstrual pad could alert you to hidden health issues like endometriosis, or even cancer. This is the promise of MenstruAI, a groundbreaking "smart pad".
What Is MenstruAI?
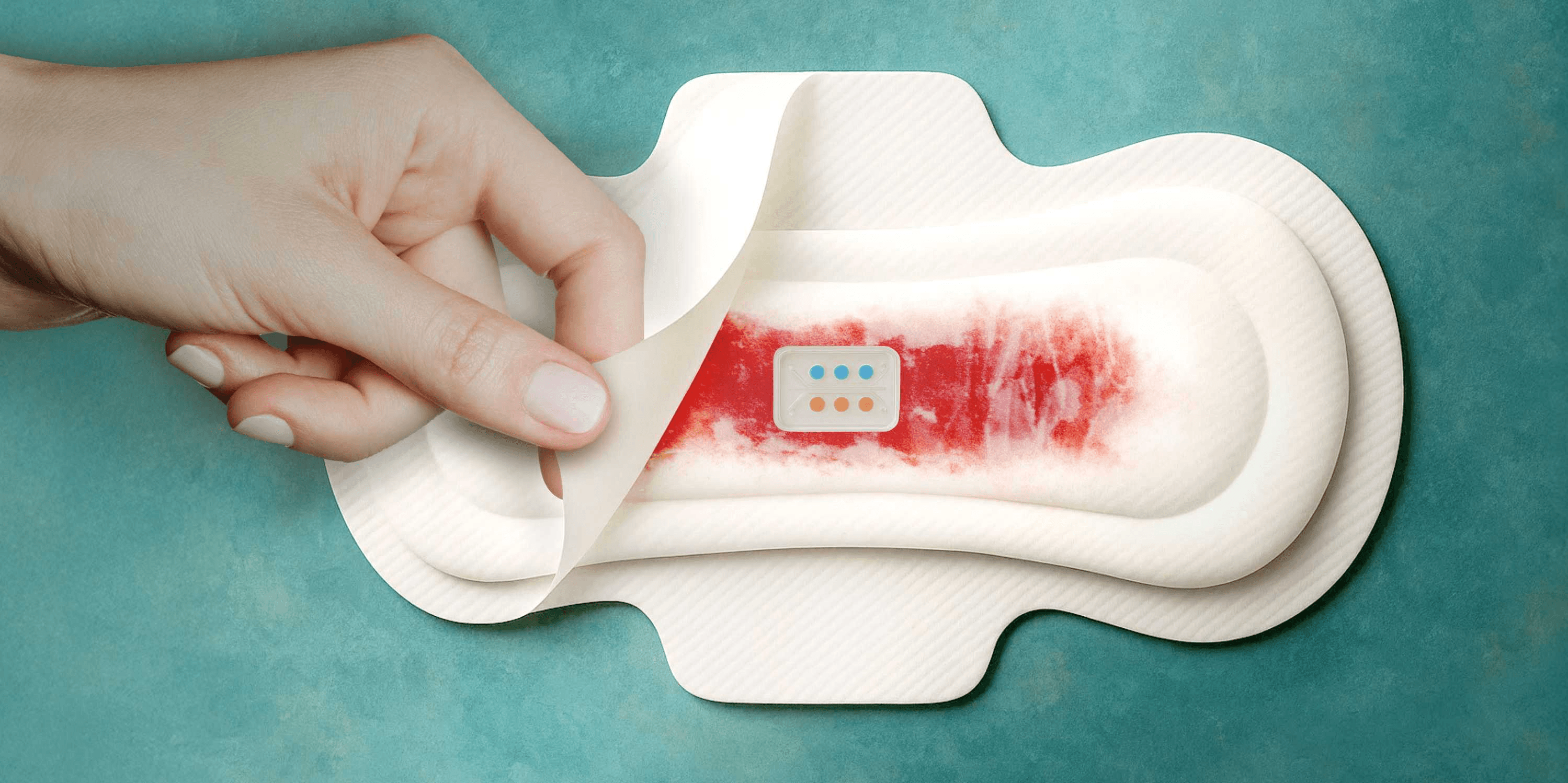
MenstruAI is a sanitary pad embedded with a lateral flow assay (LFA) paper-based biosensor, similar to a pregnancy test strip. It detects specific biomarkers in menstrual blood, such as:
C-reactive protein (CRP): Indicates inflammation or infection.
Carcinoembryonic antigen (CEA): A general tumour marker.
CA-125: Linked to ovarian cancer and endometriosis.
How Does MenstruAI Work?
Biomarkers in menstrual blood → pad’s sensor detects biomarkers → sensor triggers reaction → visible colour change appears → user interprets colour change visually or via smartphone app.
The goal is to provide a non-invasive and accessible way to monitor health and flag potential issues.
Validity and Reliability of MenstruAI
Validity
Biomarker Detection:
Laboratory and prototype testing have shown that the device can accurately and semi-quantitatively detect these biomarkers in unprocessed menstrual blood.
Clinical Relevance:
The biomarkers detected are clinically relevant for conditions like inflammation, infection, and certain gynaecological cancers.
The platform is not intended to replace clinical diagnosis but to alert users to potential health issues that may warrant further medical follow-up.
Not for All Conditions:
MenstruAI is not designed or validated to diagnose PMS (premenstrual syndrome) or PCOS (polycystic ovary syndrome), as there are no specific menstrual blood biomarkers for these conditions.
Reliability
Accuracy and Precision:
In prototype testing, MenstruAI achieved high accuracy, precision, and recall for biomarker detection (e.g., accuracy up to 0.90, precision over 0.93 when using machine learning-assisted analysis).
The device uses a lateral flow assay (LFA) platform with integrated volume control to ensure reproducibility and prevent test invalidation due to overflow.
User Experience:
The device is reported to be comfortable and indistinguishable from standard pads by users.
Results can be read visually or via a smartphone app for more precise interpretation.
How to Use MenstruAI (Based on Prototypes)
Step order | What you do | What it means in practice |
|---|---|---|
1 | Select a pad | Choose one that matches your flow (light or heavy). |
2 | Position the pad | Stick it onto your underwear like a regular pad. |
3 | Wear as usual | Go about your day; the sensor stays discreet. |
4 | Check results – visual read | Look at the pad and compare color to the chart. |
5 | Check results – app scan | Use the smartphone app to scan for exact levels. |
6 | Dispose safely | Wrap the used pad and throw it in the trash. |
7 | Follow up if needed | Contact a doctor if the results look abnormal. |
What Can MenstruAI Actually Detect?
Inflammation and Infection (CRP)
MenstruAI can detect elevated CRP levels, which may indicate inflammation or infection in the body. This could prompt users to seek medical advice if something seems amiss.
Cancer Markers (CEA, CA-125)
The device can also detect CEA and CA-125, which are associated with certain cancers (like ovarian or colorectal cancer) and conditions like endometriosis. However, these markers are not specific to any one disease and can be elevated for many reasons, including normal menstrual variation.
Endometriosis (CA-125)
CA-125 is sometimes elevated in people with endometriosis, but it is not a definitive diagnostic tool. Many other factors can raise CA-125 levels, so a positive result would require further clinical evaluation.
Limitations of MenstruAI
1. Narrow Biomarker Range
MenstruAI focuses on CRP, CEA, and CA-125. It cannot detect:
Hormones (e.g., estrogen, testosterone) critical for diagnosing PCOS.
Metabolic markers (e.g., insulin resistance) linked to PCOS.
2. Not a Diagnostic Tool
Screening vs. diagnosis: MenstruAI alerts users to abnormalities but can’t confirm diseases. Elevated CA-125, for example, could mean endometriosis—or just normal menstrual variation.
Requires clinical follow-up: Any abnormal result must be verified through blood tests, imaging, or biopsies.
3. Technical Challenges
Flow variability: Heavy periods can flood the sensor, skewing results.
User error: Misinterpreting colour changes or app glitches could lead to false alarms.
4. Early-Stage Technology
Prototype phase: Most data comes from lab tests or small trials. Large-scale validation is lacking.
Not peer-reviewed: Key studies are preprint papers, not yet vetted by independent experts.
5. Privacy Concerns
Data security: Health data collected via smartphone apps could be vulnerable to breaches.
6. Not Widely Available:
MenstruAI is not yet FDA-approved or available for general consumer use
Conclusion
MenstruAI and similar “smart pads” are pioneering a new approach to women’s health by analyzing menstrual blood for certain biomarkers offering a non-invasive way to monitor certain health markers in menstrual blood. It is reliable for the biomarkers it targets, easy to use, and comfortable. However, their capabilities are limited: they can screen for inflammation, infection, and some cancer markers, but they cannot diagnose PMS or PCOS. Tracking your cycle alongside mood changes using apps such as HealCycle can help manage and understand conditions like PMDD.
Disclaimer
MenstruAI is not FDA-approved and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult a healthcare provider for health concerns.
References
Preti, A. et al. (2023). MenstruAI: A Smart Pad for Women’s Health Monitoring (preprint).
American College of Obstetricians and Gynecologists. (2023). Polycystic Ovary Syndrome (PCOS).
Munro, M. G., Critchley, H. O. D., & Fraser, I. S. (2024). The menstrual cycle as a vital sign: A comprehensive review. Current Opinion in Obstetrics & Gynecology, 36(1), 1–9.
Reed, B. G., & Carr, B. R. (2023). Physiology, menstrual cycle.
Critchley, H. O. D., Babayev, E., Bulun, S. E., Clark, S., Garcia-Grau, I., Gregersen, P. K., Kilcoyne, A., Kim, J. J., Lavender, M., Marsh, E. E., Matteson, K. A., Maybin, J. A., Metz, C. N., Moreno, I., Silk, K., Sommer, M., Simon, C., Tariyal, R., Taylor, H. S., Wagner, G. P., Griffith, L. G., & Mullin, G. E. (2020). Menstruation: Science and society.
American Journal of Obstetrics and Gynecology, 223(5), 624–664.Chen, J., Yu, J., Li, X., Zhang, X., & Dai, X. (2024). Menstrual health under the scientific microscope: Text mining analysis. Women’s Health, 20, 17455057241290895
Hennegan, J., Shannon, A. K., Rubli, J., Schwab, K. J., & Melendez-Torres, G. J. (2020). Measurement in the study of menstrual health and hygiene: A systematic review and audit. PLOS ONE, 15(6), e0232935.
Latest
From the Blog
Discover fresh insights, practical tips, and empowering stories to help you learn and grow in your PMDD healing journey. We're always here to remind you that you're not alone




